Tooth extraction seems as a painful and complicated procedure to most of the patients. However, it is a completely painless operation since it is performed under local anesthesia. Moreover, today, there are plenty of special instruments and techniques that simplify the procedure to a great extent.
Nevertheless, there are cases where tooth extraction may become more challenging. Thus, for instance, when a tooth is destroyed bellow the gum level or is impacted (fully or partially covered by the jaw bone) then a surgical procedure may be necessary in order to extract the tooth. In these cases, and again under local anesthesia, the gums surrounding the tooth are pushed back allowing the dentist to gain better access to remove the tooth. Right after the surgical extraction sutures are placed in order to bring the gums back together and thus help the healing process. The teeth that are more often extracted surgically, are the wisdom teeth, due to the fact that most of the times they are impacted. Without a doubt, the experience of the dentist is of critical importance for the smooth extraction of this type of teeth.
- suffer from diabetes have to undergo an extraction procedure when the sugar levels in their blood are within normal range. Thus the time of the day when an extraction should be performed may vary depending upon the prescribed medication and their diet.
- take anticoagulants may have to stop receiving their medication a few days before the extraction or modify their anticoagulant therapy (i.e receive heparin). These changes may prevent hemorrhage and must be performed only according to the instructions provided by the patient’s cardiologist.
- suffer from valvulopathy or have undergone arthroplasty or have a heart stent must take antibiotics prior to extraction. Usually these patients receive prophylactic antibiotics an hour before the procedure, according to the instructions provided by their cardiologist or orthopedic doctor.
- suffer from high blood pressure should undergo tooth extraction using a local anesthetic with low concentration in adrenaline.
- have allergies on specific painkillers or anti-inflammatory drugs or antibiotics, must follow a different prescribed medication if the dentist considers it necessary.
It is clear, that if the patient suffers from a serious health problem, the dentist may ask for additional clinical examinations or refer the patient to a physician in order to address the medical problem first.
After tooth extraction the patient should follow the instructions bellow:
- Place an ice-pack outside of the mouth next to the extraction site. Remove the ice-pack for a few minutes every 10 minutes for the next 4 hours. The ice-pack will reduce the swelling.
- Do not spit.
- Put pressure with a small gauze on the extraction site for half an hour.
- Avoid smoking during the healing period.
- Pain-killers, anti-inflammatory drugs or antibiotics, have to be taken according to the instructions provided by the dentist.
- If a short-range hemorrhage incident occurs during the healing process, put pressure with a small wet gauze on the extraction site. If there are large blood clots you should contact your dentist for further instructions.
- The swelling is not something uncommon and subsides in 3-7 days. If it appears 3-4 days after the extraction procedure you should contact your dentist.
- The day of the extraction try to avoid brushing your teeth. From the day-two brush softly all the teeth apart from the extraction site, rinse with a mouthwash 3 times a day for 7-10 days.
- If stitches have been placed, they will be removed 7-10 days after the extraction. Do not touch the stitches with your tongue. In case a stitch gets loose you should contact your dentist.
- The first two days after extraction, you should drink and eat only cold beverages and foods. You should drink fluids and be on a soft diet for the next 7 days. You should always chew away from the extraction area.
These are some general guidelines for the post-extraction period. If the dentist has provided individualized recommendations it goes without saying that you have to follow them
- Pain. Is most intense same day the extraction took place and particularly right after anesthesia wears out.
- Swelling. This is quite common and may extend to the surrounding tissues. To reduce the likelihood of swelling to occur, the patient should place on the cheek an ice-pack for 3-4 hours, periodically.
- Hemorrhage. If such a case occurs, it is recommended that you press the extraction area with a wet gauze for 30 minutes. Furthermore, for minimizing the possibility of a new hemorrhage incident, you should avoid the intense physical exercise and not chew food on the sensitive area.
- Hematoma. A less common phenomenon after extraction is the development of a hematoma in the cheek region. This kind of hematoma will be absorbed in a period of 1-2 weeks. The hematoma changes its color from dark brown to light yellow and will fade out with time.
- Dry socket. If during the healing period the blood clot is removed from the socket, then the bone of the jaw gets exposed and dries out leading to a dry socket. This is accompanied with acute pain for 2 weeks. If a dry socket occurs, then the patient must visit the dentist in order to have a soothing substance placed in the socket (eugenol). This procedure may need to be repeated for the next few days. To reduce the risk of a dry the patient should not suck out and spit out the blood clot that has been formed in the socket. Additionally, smoking should be avoided during the healing period.
- Oral-sinus communication. There are a few cases where the roots of the upper posterior teeth are located inside the sinus cavities. Thus, the extraction of those teeth may lead to the communication of the oral and sinus cavities. The dentist is expected to diagnose such a case when the extraction takes place and address the problem. Otherwise, there is a high risk of developing an inflammation in the sinus area that needs to be treated immediately.
Despite these general guidelines, if the patient notices something going wrong during the healing period, then he/she should inform his/her dentist immediately.
The presence of impacted teeth can cause a variety of problems both aesthetic and functional. Specifically, when a tooth is missing from the occlusion, an empty space is created that apart from the aesthetic appearance, restrains the chewing ability of the patient. Moreover, the adjacent teeth move into the empty spot resulting in the distortion of the correct occlusion of the teeth. Finally, the presence of an impacted tooth is an impediment to the placement of an implant aiming at filling the empty spot.
In order for these problems to be resolved, the exposure of these teeth is mandatory. Thus, with a small surgical procedure the dentist can expose the impacted tooth and with the help of orthodontics may move the tooth to it correct place.
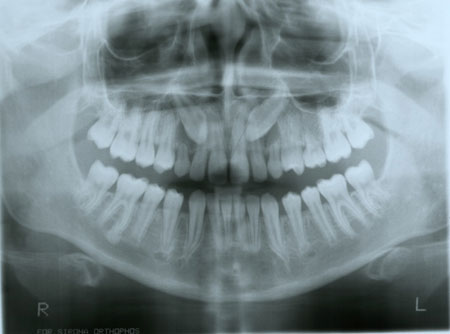
Impacted canine teeth in the upper jaw
- They are not oriented correctly, resulting in their inability to emerge to the right place in the mouth.
- There isn’t enough capacity for the teeth to emerge to the right place. This is usually an issue when the deciduous teeth are lost in an earlier age than expected and the adjacent teeth have been moved and have covered the space intended for the impacted tooth.
- The gums are too thick and too firm interferes with the normal emergence of the tooth.
- The tooth is integrated with the jaw bone (attached).
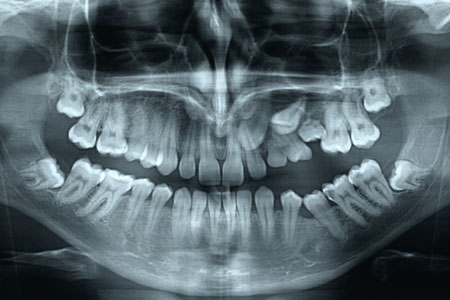
Περιστατικό
- Case / Impacted teeth in the upper jaw bone
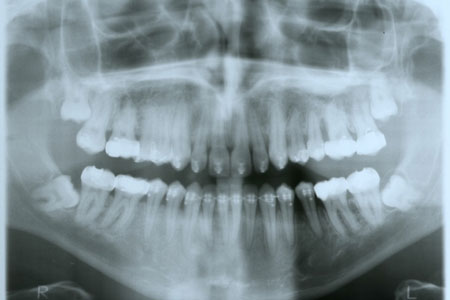
- After exposure and orthodontic movement in the right place
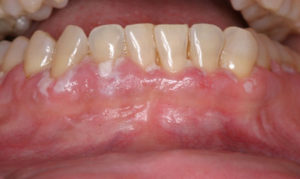
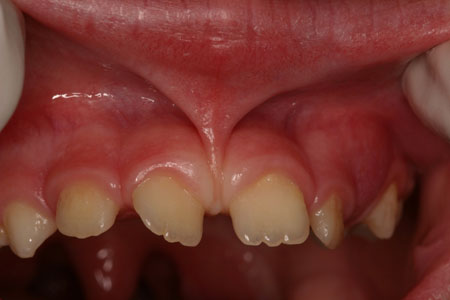
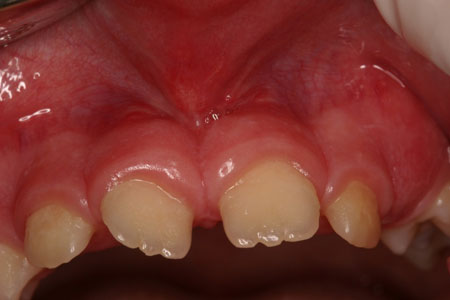
The lip frenum is a fold of the mucous membrane that partially connects the lip with gums. The presence of the frenum is not mandatory for the support of the lip. Thus, when the anatomy of the frenum is such that causes problems, the dentist can decide to remove it through a procedure called frenectomy. Frenectomy is a simple surgical procedure that takes place under local anaesthesia without causing any particular post-surgical discomfort and deals with the problem permanently.
- Before frenectomy
- After frenectomy
- if it is hypertrophic and causes an aesthetic problem.
- If it binds high on the gum boundary and interferes with effective oral hygiene.
- If it interferes with an area that there is a gum recession and the root of the tooth has been exposed.
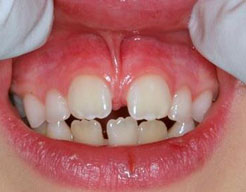
- If it is hypertrophic and interferes between the teeth, separating them and creating a gap between them.
Some oral lesion can be the first signs of a systemic disease or even of oral cancer especially in smokers and people that are frequently exposed to sun light. Therefore, patients need to inform immediately their dentist when something unusual appears in their mouth. It is certain that the early diagnosis can minimized the need for extensive treatment.